Introduction
Re-credentialing is a routine yet critical aspect of maintaining compliance and payer relationships. However, the process can quickly become overwhelming, with multiple providers, payers, and deadlines to manage. Failing to stay on top of re-credentialing requirements can lead to delisting, billing interruptions, and compliance penalties.
In this blog, we’ll explore strategies to simplify re-credentialing, ensuring your practice stays compliant and operates smoothly without unnecessary stress.
The Importance of Re-Credentialing
- Ensures Compliance with Payer Requirements
Payers require regular re-credentialing to verify provider qualifications and maintain network standards. - Prevents Revenue Interruptions
Missing re-credentialing deadlines can result in temporary delisting, delaying claims and reimbursements. - Supports Patient Access
Maintaining active credentials ensures uninterrupted patient access to your services. - Protects Your Practice During Audits
Accurate and up-to-date credentials are essential for passing payer and regulatory audits.
Common Challenges in Re-Credentialing
- Tracking Multiple Deadlines
- Challenge: Different providers and payers have varying timelines, making it difficult to stay organized.
- Solution: Implement a centralized system to monitor all upcoming deadlines.
- Managing Complex Documentation
- Challenge: Providers must submit updated licenses, certifications, and insurance, which can be time-consuming to gather.
- Solution: Use a credentialing platform to store and update documentation securely.
- Lack of Communication with Payers
- Challenge: Delayed responses from payers can stall the re-credentialing process.
- Solution: Establish clear communication channels with payer representatives to address issues promptly.
- Staff Turnover or Resource Constraints
- Challenge: Changes in your credentialing team or limited staff capacity can cause gaps in the re-credentialing process.
- Solution: Develop standardized workflows and provide ongoing training to ensure continuity.
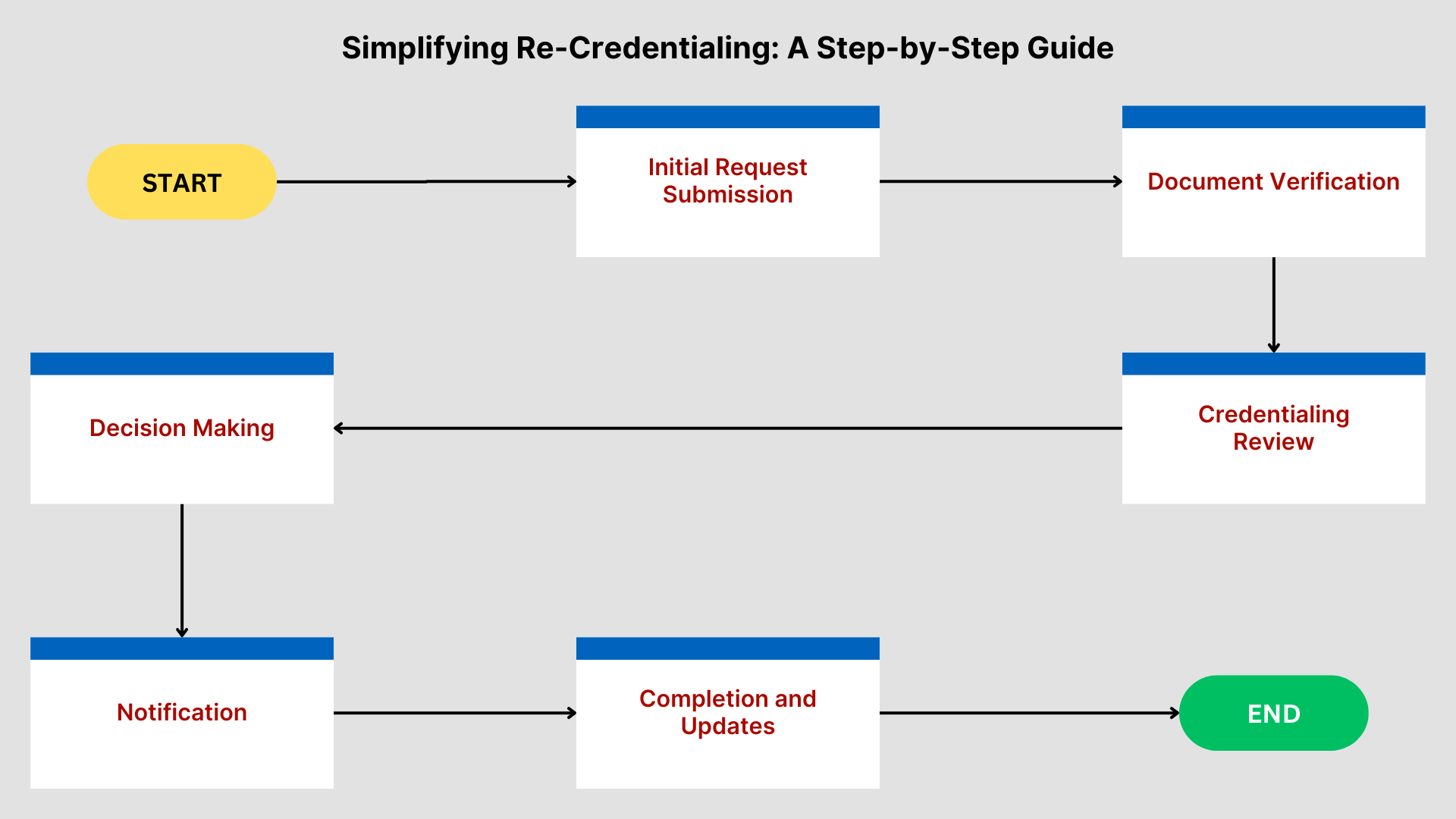
Strategies to Simplify Re-Credentialing
- Centralize Credentialing Records
- Why It Works:
Ensures all necessary documents are easily accessible and up to date. - How to Do It:
Use a credentialing management system to store licenses, certifications, and payer-specific forms securely.
- Why It Works:
- Automate Deadline Tracking
- Why It Works:
Reduces the risk of missed deadlines and ensures timely submissions. - How to Do It:
Set up automated reminders and notifications for upcoming re-credentialing requirements.
- Why It Works:
- Conduct Regular Internal Audits
- Why It Works:
Identifies gaps in provider files and resolves issues before they impact re-credentialing. - How to Do It:
Schedule quarterly reviews of all credentialing records to catch expired or missing documents.
- Why It Works:
- Streamline Communication with Payers
- Why It Works:
Minimizes delays caused by incomplete or unclear submissions. - How to Do It:
Assign dedicated staff to liaise with payers and resolve issues quickly.
- Why It Works:
- Standardize Workflows for Consistency
- Why It Works:
Reduces errors and ensures all team members follow the same process. - How to Do It:
Create a step-by-step re-credentialing guide for your team to follow.
- Why It Works:
Not all payers are equal in terms of revenue impact. Focus on timely re-credentialing for high-value payers first to ensure minimal disruption to your cash flow.
How WWS Can Help
At WWS, we take the stress out of re-credentialing with tailored solutions:
- Centralized Systems: Our credentialing platforms streamline document management and deadline tracking.
- Automated Reminders: Never miss a re-credentialing deadline with our automated notification tools.
- Payer Expertise: We handle payer communications and resolve issues quickly to keep your practice compliant.
Schedule a consultation with WWS today to simplify your re-credentialing process:
Schedule a Meeting with WWS.
Conclusion
Re-credentialing doesn’t have to be a source of stress for your team. By centralizing records, automating processes, and maintaining clear communication with payers, you can simplify the process and stay compliant with minimal effort.
Partner with WWS to streamline your re-credentialing and maintain compliance—schedule your consultation today!




