Answer Summary
Generic emails delay contracts by creating context gaps that force payer representatives to manually search for provider data, often resulting in automated “wait 60 days” responses rather than file progress. Implementing a “Context-First” protocol with specific subject lines and proactive status requests can reduce administrative turnaround by 15% and is critical for maintaining 2026 CMS compliance standards for timely provider credentialing. By shifting from passive inquiries to authoritative, data-backed follow-ups, DME providers remove operational friction and accelerate their path to billable status.
The Scenario: The Black Hole of Communication
On January 24th, the Provider Enrollment team submitted a Letter of Interest (LOI) to a major payer, “SCAN Health Plan,” for a provider named “Opry Medical Group” (anonymized). The initial submission was standard. The automated receipt arrived. The clock started ticking.
Three days later, a team member named “William Thomas” sent a follow-up: “It is a pleasure to receive this update. I am looking forward to hearing from you again.”
Two months later, on March 20th, William sent another email: “Could you please provide us with any updates on our request?”
The result? A polite but useless response from the payer: “Please allow up to 60 days for a decision”. The application had stalled for 55 days with zero meaningful progress.
The Operational Failure
This case study highlights a subtle but expensive failure mode: Vague Communication.
1. The Context Gap
When William asked for “updates on our request,” he assumed the payer rep knew who he was. He didn’t include the Provider Name, the NPI, or the Submission Date in his subject line or opening sentence. For a payer rep handling thousands of emails, this “mystery email” requires them to stop, search their database by the sender’s email address, and try to guess which file is being referenced.
Our analysis estimates this lack of context wasted 30 minutes per email in back-and-forth clarification.
2. The “Canned Response” Trigger
By sending a generic “Any update?” email, the team essentially invited a generic “Wait 60 days” response. There was no specific question or “Call to Action” that forced the payer rep to actually look at the file.
3. Thread Hygiene
The team kept replying to the same email thread for months, burying the original submission details under layers of signatures and disclaimers. This made the email history “cluttered” and difficult to scan.
The WWS Solution: Context-First Protocol
To fix this, WWS completely overhauled the team’s email templates. We introduced the “Context-First” Protocol.
1. The “Smart” Subject Line
We banned generic subject lines like “Follow Up.” The new standard is:
- [Provider Name] – Submitted [Date] – LOI Status Update
- Example: Opry Medical Group – Submitted Jan 24 – Status Update
This allows the payer rep to locate the file before they even open the email.
2. The Proactive Narrative
We rewrote the body copy to be specific and authoritative. Instead of asking “Any updates?”, the new script reads:
“It has been 8 weeks since our submission on January 24th. Given your standard 60-day review window, we are requesting a status confirmation today.”
This shows the payer that we are tracking the timeline and holding them accountable.
3. Proactive Information Gathering
We trained the team to anticipate the payer’s needs. Instead of waiting to be asked for documents, the follow-up emails now proactively confirm: “We have verified that our CAQH profile is current as of [Date] to expedite your review.”
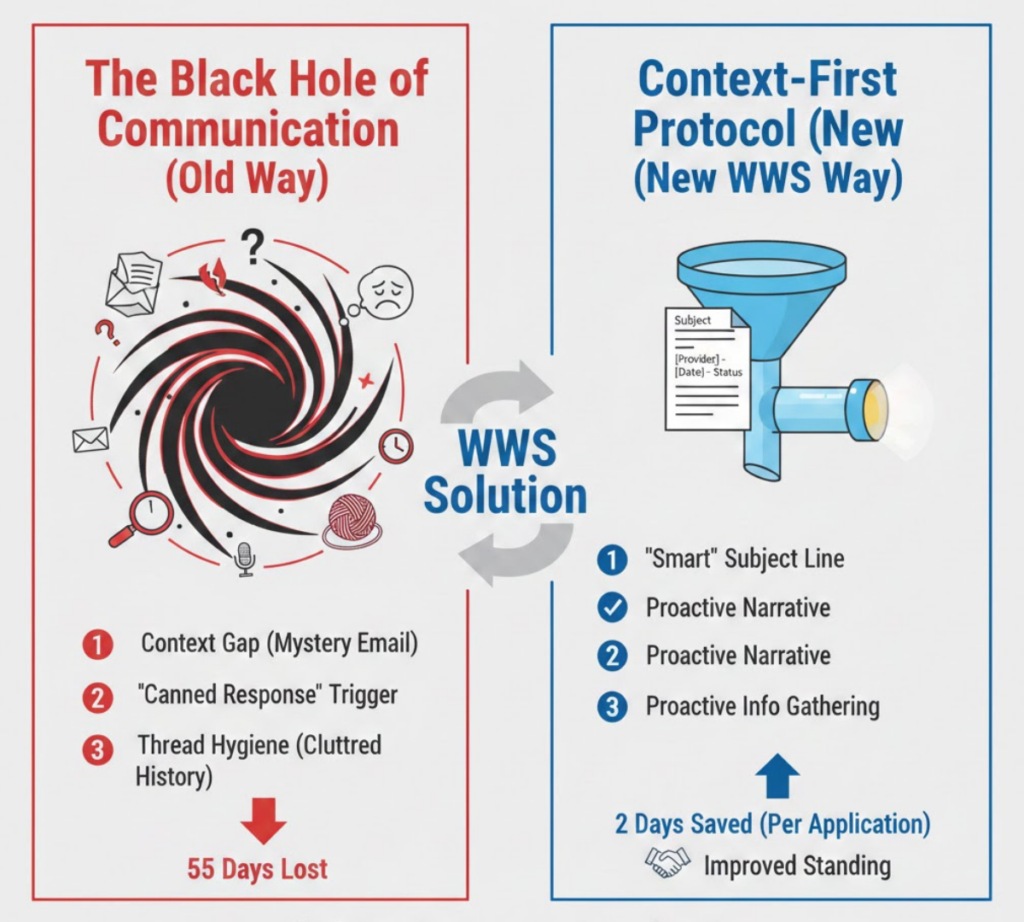
The Outcome
Clarity is currency. By removing the friction for the payer rep, we reduced the administrative turnaround time by 2 days per application. More importantly, the tone shift from “passive requester” to “active manager” improved our professional standing with payer representatives.




