Introduction
Credentialing is a complex, time-consuming process that requires precision, attention to detail, and up-to-date knowledge of payer and regulatory requirements. For many DME providers, managing credentialing in-house can strain resources and lead to errors. Outsourcing credentialing offers an alternative that can streamline workflows, reduce administrative burden, and enhance compliance—but is it the right choice for your practice?
In this blog, we’ll explore the benefits, considerations, and potential challenges of outsourcing credentialing, helping you decide if it’s the right solution for your DME practice.
Why Consider Outsourcing Credentialing?
- Reduce Administrative Burden
Credentialing involves extensive paperwork, tracking, and communication with payers. Outsourcing these tasks allows your team to focus on patient care and other priorities. - Enhance Accuracy and Compliance
Credentialing experts stay updated on payer requirements and industry regulations, minimizing errors and ensuring compliance. - Improve Efficiency
Outsourced providers leverage advanced tools and workflows to accelerate approvals and renewals. - Access Expertise
Credentialing firms bring specialized knowledge and established relationships with payers, streamlining the process. - Scale with Your Practice
As your practice grows or expands into new states, outsourcing offers the flexibility to manage increased credentialing demands without adding internal staff.
Key Considerations Before Outsourcing
- Evaluate Your Current Workflow
- Questions to Ask:
- Is your in-house team consistently meeting credentialing deadlines?
- Are errors or delays impacting reimbursements?
- What to Do:
Assess the effectiveness of your current processes to identify gaps outsourcing could fill.
- Questions to Ask:
- Assess Costs vs. Benefits
- Questions to Ask:
- How does the cost of outsourcing compare to maintaining or expanding your in-house team?
- Will outsourcing free up resources that can be reallocated to other priorities?
- What to Do:
Calculate potential cost savings, including reductions in administrative workload and denial rates.
- Questions to Ask:
- Choose the Right Partner
- Questions to Ask:
- Does the outsourcing provider specialize in DME credentialing?
- Can they handle payer-specific and state-specific requirements?
- What to Do:
Look for credentialing firms with proven expertise, robust technology, and strong client references.
- Questions to Ask:
- Consider Control and Transparency
- Questions to Ask:
- How much control will you retain over the credentialing process?
- Will the outsourcing provider offer real-time updates and reporting?
- What to Do:
Ensure your outsourcing partner provides clear communication and accessible metrics.
- Questions to Ask:
- Plan for Collaboration
- Questions to Ask:
- How will the outsourcing team collaborate with your internal staff?
- Are workflows and responsibilities clearly defined?
- What to Do:
Develop a partnership model that integrates outsourced services with your existing operations.
- Questions to Ask:
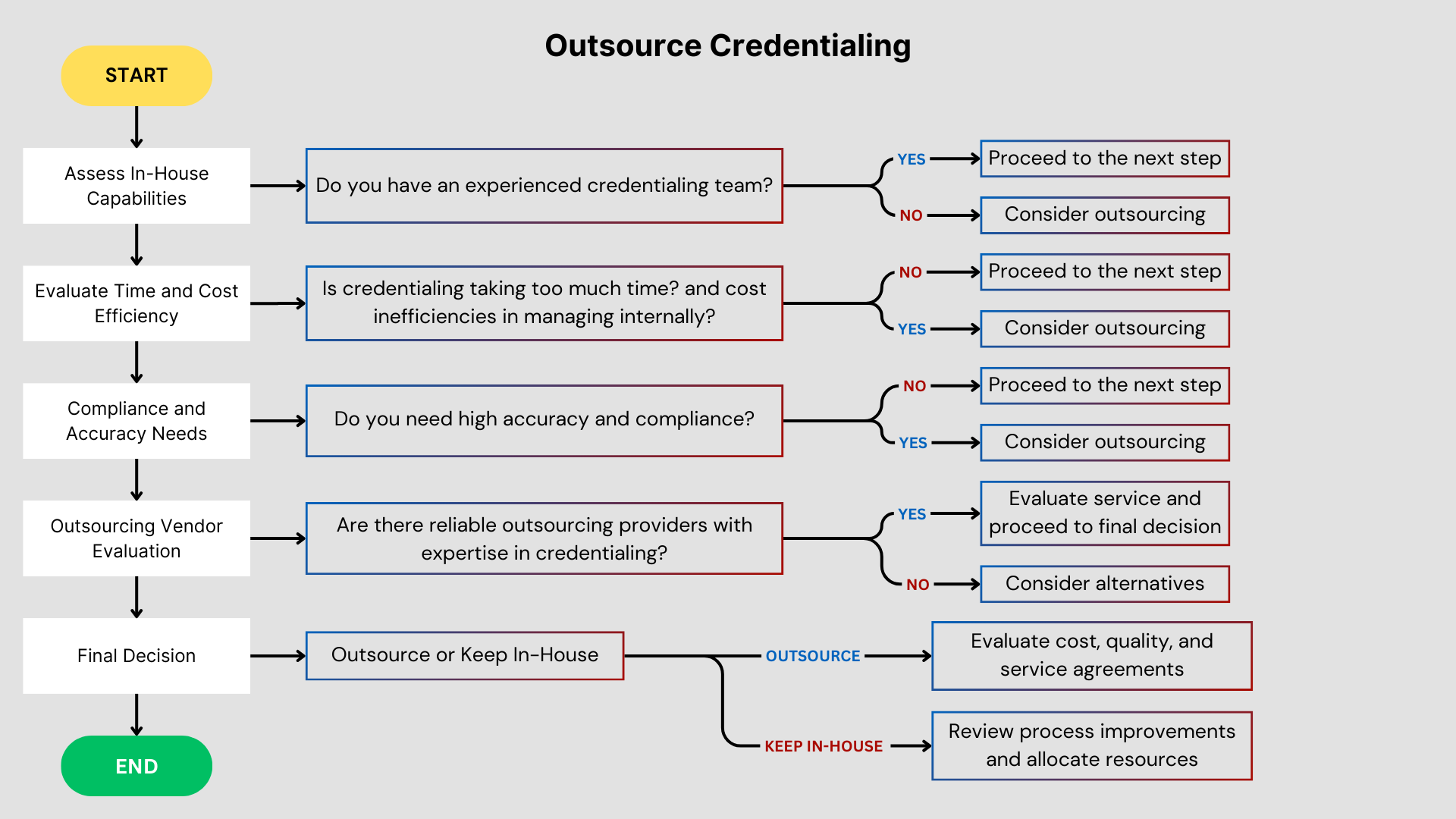
Potential Challenges of Outsourcing Credentialing
- Loss of Immediate Oversight
Relying on an external provider may reduce your ability to monitor day-to-day credentialing activities. - Integration with Existing Systems
Outsourcing providers need access to your documentation and billing platforms, which can require initial setup and adjustments. - Vendor Reliability
Choosing the wrong partner could lead to miscommunication, delays, or lack of transparency.
How to Make Outsourcing Work for Your DME Practice
- Set Clear Expectations
Define roles, responsibilities, and performance metrics in your agreement with the outsourcing provider. - Prioritize Communication
Establish regular check-ins and reporting to ensure transparency and address concerns promptly. - Monitor Performance
Track key metrics like approval timelines, renewal rates, and error reductions to evaluate the provider’s effectiveness. - Start Small
Consider outsourcing a portion of your credentialing workload (e.g., new provider onboarding) before transitioning fully. - Maintain Access to Critical Data
Ensure all credentialing documentation remains securely accessible to your practice, even when managed externally.
How WWS Can Help
At WWS, we offer comprehensive outsourcing solutions designed for DME providers:
- Tailored Workflows: We customize our processes to align with your specific needs and payer requirements.
- Advanced Technology: Our platforms streamline credentialing, ensuring accuracy and compliance at every step.
- Transparent Communication: You’ll have access to real-time updates and detailed reports on your credentialing status.
- Proven Expertise: With deep knowledge of DME credentialing, we handle complex payer requirements and regulatory challenges with ease.
Schedule a consultation with WWS today to explore outsourcing options for your practice:
Schedule a Meeting with WWS.
Conclusion
Outsourcing credentialing can be a game-changer for DME providers, offering efficiency, accuracy, and scalability. However, it’s essential to evaluate your needs, choose the right partner, and maintain oversight to ensure success.
Partner with WWS to streamline your credentialing process—schedule your consultation today!




