Introduction
Internal credentialing audits are an essential practice for DME providers, ensuring compliance with payer and regulatory standards while reducing the risk of errors and penalties. A well-executed audit not only identifies gaps in your processes but also helps streamline operations and improve overall efficiency.
In this blog, we’ll walk you through the steps to conduct an effective internal credentialing audit, highlighting best practices and tools to maintain compliance and avoid disruptions.
Why Conduct an Internal Credentialing Audit?
- Ensure Compliance
Regular audits verify that your credentialing files meet payer, state, and federal requirements. - Reduce Risk of Penalties
Identifying and resolving gaps proactively can help you avoid fines, delisting, or failed payer audits. - Improve Workflow Efficiency
Audits highlight bottlenecks and inefficiencies in your credentialing processes, allowing for targeted improvements. - Strengthen Payer Relationships
Maintaining accurate and up-to-date records builds trust and minimizes disputes with payers. - Prepare for External Audits
Internal audits serve as a practice run, ensuring your team is ready for official payer or accreditation reviews.
Key Areas to Focus On During a Credentialing Audit
- Provider Documentation
- What to Review:
Licenses, certifications, insurance, and any payer-specific forms. - Common Issues:
Missing, expired, or inaccurate records.
- What to Review:
- Compliance with Payer Requirements
- What to Review:
Adherence to credentialing timelines and payer-specific standards. - Common Issues:
Incomplete applications or failure to meet submission deadlines.
- What to Review:
- Credentialing Timelines
- What to Review:
Time taken to complete initial credentialing and re-credentialing. - Common Issues:
Delays in submissions leading to interruptions in billing or network participation.
- What to Review:
- Integration with Billing
- What to Review:
Credentialing status of providers linked to claims submissions. - Common Issues:
Claims submitted for uncredentialed providers resulting in denials.
- What to Review:
- Internal Processes and Training
- What to Review:
Workflow consistency and team adherence to credentialing protocols. - Common Issues:
Staff errors due to inadequate training or unclear procedures.
- What to Review:
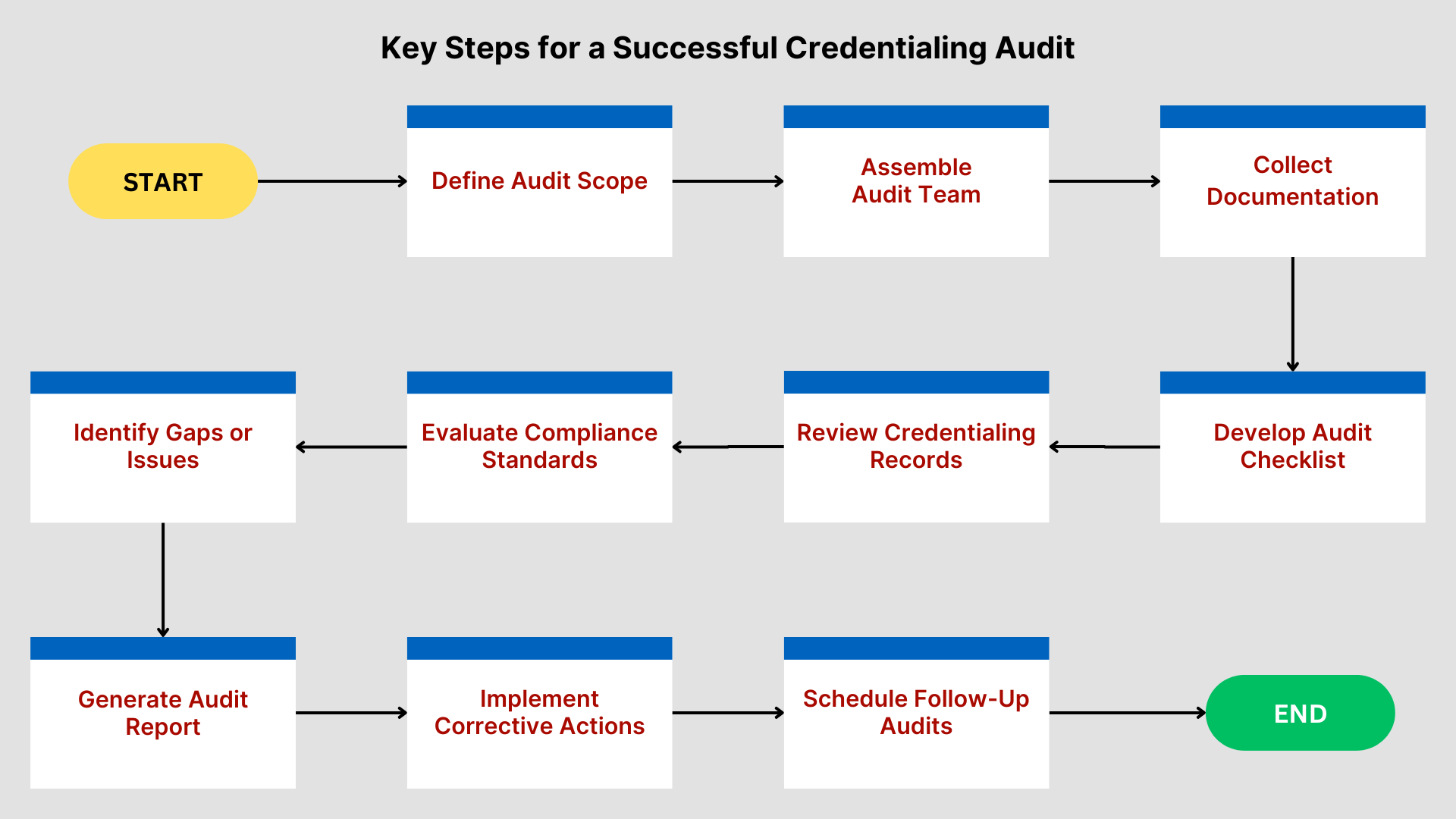
Steps to Conduct an Effective Credentialing Audit
- Define Audit Objectives
- Why It Works:
Clear objectives ensure the audit focuses on the most critical areas. - How to Do It:
Identify goals, such as verifying compliance, improving efficiency, or preparing for an external review.
- Why It Works:
- Create an Audit Checklist
- Why It Works:
A comprehensive checklist ensures no key areas are overlooked. - How to Do It:
Include items like provider documentation, payer-specific requirements, and internal workflows.
- Why It Works:
- Gather and Organize Data
- Why It Works:
Centralized records make it easier to review credentialing files systematically. - How to Do It:
Use credentialing software to collect and organize provider data before the audit.
- Why It Works:
- Conduct the Review
- Why It Works:
A thorough review identifies gaps and inconsistencies. - How to Do It:
Compare provider files against payer requirements, ensuring all documentation is complete and accurate.
- Why It Works:
- Document Findings and Prioritize Issues
- Why It Works:
Detailed findings help you address the most critical gaps first. - How to Do It:
Categorize findings by severity and create an action plan to resolve high-priority issues.
- Why It Works:
- Implement Corrective Actions
- Why It Works:
Resolving gaps ensures compliance and prevents future errors. - How to Do It:
Update missing documents, retrain staff, or revise workflows as needed.
- Why It Works:
- Monitor and Follow Up
- Why It Works:
Continuous monitoring ensures long-term compliance and efficiency. - How to Do It:
Schedule regular follow-ups to track progress on corrective actions and refine processes.
- Why It Works:
Credentialing software can automate data collection, organize files, and generate reports, saving time and reducing errors during audits.
How WWS Can Help
At WWS, we simplify the credentialing audit process with tailored solutions for DME providers:
- Audit Preparation Tools: Our systems centralize records and automate tracking to streamline audits.
- Expert Guidance: We provide checklists, best practices, and actionable insights for conducting effective audits.
- Corrective Action Support: Our team helps you resolve gaps and implement improvements for long-term compliance.
Schedule a consultation with WWS today to enhance your credentialing audit process:
Schedule a Meeting with WWS.
Conclusion
Internal credentialing audits are a proactive way to ensure compliance, streamline workflows, and reduce risk. By focusing on key areas, leveraging technology, and addressing gaps promptly, your practice can maintain smooth operations and strengthen payer relationships.
Partner with WWS to streamline your credentialing audits and stay ahead of compliance requirements—schedule your consultation today!




