Introduction
Securing new payer contracts is a significant milestone for DME providers, offering opportunities to expand patient access and increase revenue. However, credentialing for new contracts often presents challenges, from navigating payer-specific requirements to meeting tight deadlines. Proper preparation and a strategic approach can simplify the process and ensure timely approval.
In this blog, we’ll outline best practices for credentialing under new payer contracts, helping you streamline the process and establish strong payer relationships from the start.
Why Credentialing for New Payer Contracts Is Critical
- Expands Revenue Opportunities
Credentialing ensures you can start billing the payer and accessing new patient populations promptly. - Strengthens Payer Relationships
Efficient credentialing builds trust with payers and sets the tone for a successful partnership. - Avoids Billing Delays
Completing credentialing before providing services prevents claim denials and payment interruptions.
Common Challenges in Credentialing for New Payer Contracts
- Navigating Payer-Specific Requirements
- Challenge: Each payer has unique credentialing standards, making it difficult to standardize the process.
- Solution: Develop payer-specific checklists to ensure compliance with individual requirements.
- Tight Deadlines
- Challenge: Delays in credentialing can push back your billing start date, affecting revenue.
- Solution: Use automation to track deadlines and prioritize high-value contracts.
- Gathering Complete Documentation
- Challenge: Missing or incorrect documents can result in application rejections and extended timelines.
- Solution: Centralize provider records in a credentialing platform to simplify document collection and updates.
- Payer Communication Barriers
- Challenge: Inconsistent communication with payer representatives can stall the credentialing process.
- Solution: Assign a dedicated team member to liaise with payers and follow up regularly on application progress.
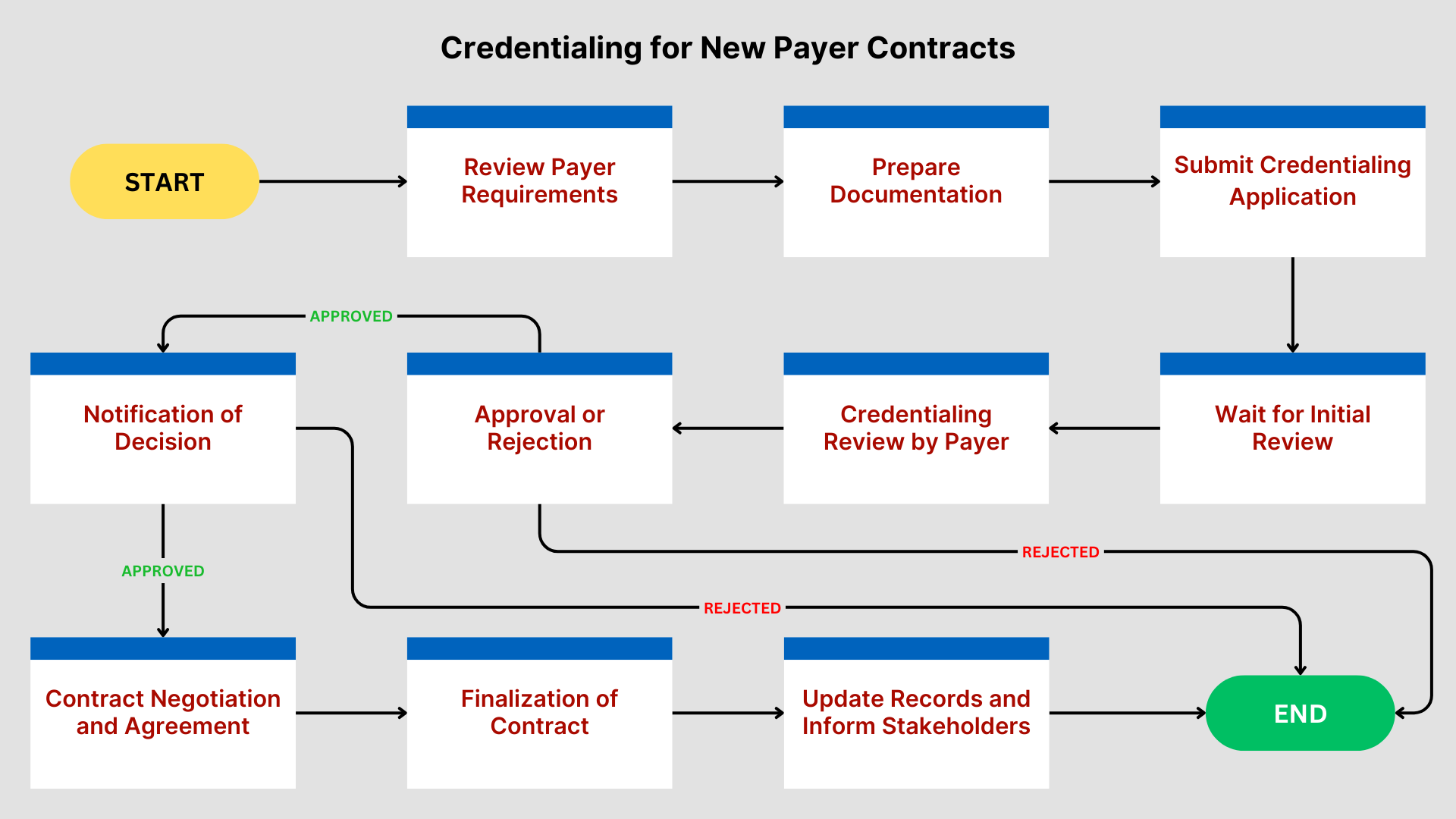
Best Practices for Credentialing Under New Payer Contracts
- Research Payer Requirements in Advance
- Why It Works:
Understanding each payer’s expectations ensures you submit complete and accurate applications. - How to Do It:
Request credentialing guides from payers and review them thoroughly before starting the process.
- Why It Works:
- Prepare a Centralized Provider Database
- Why It Works:
Easily accessible provider information accelerates application preparation and submission. - How to Do It:
Use a credentialing management system to organize and update provider records.
- Why It Works:
- Automate Documentation and Deadlines
- Why It Works:
Automation reduces manual errors and ensures you meet payer timelines. - How to Do It:
Implement tools that send reminders for missing documents and approaching deadlines.
- Why It Works:
- Create a Step-by-Step Credentialing Workflow
- Why It Works:
A structured process minimizes errors and delays, ensuring consistency across applications. - How to Do It:
Develop a checklist covering key steps, including document gathering, submission, and payer follow-ups.
- Why It Works:
- Build Strong Relationships with Payers
- Why It Works:
Positive communication with payer representatives can expedite credentialing approvals. - How to Do It:
Regularly engage with payers through emails, calls, or meetings to discuss application statuses and resolve issues promptly.
- Why It Works:
Don’t wait for the contract to be fully executed—begin gathering documentation and preparing applications as soon as negotiations are underway to shorten the onboarding timeline.
How WWS Can Help
Navigating credentialing for new payer contracts can be complex, but WWS makes it seamless:
- Payer-Specific Expertise: We understand the unique requirements of major payers and tailor workflows accordingly.
- Automation Solutions: Our tools track deadlines, organize documentation, and streamline the credentialing process.
- Payer Communication Support: We act as your liaison with payers, ensuring faster approvals and reduced delays.
Schedule a consultation with WWS today to simplify credentialing for new payer contracts:
Schedule a Meeting with WWS.
Conclusion
Credentialing for new payer contracts is essential for expanding your practice and maximizing revenue potential. By preparing thoroughly, automating processes, and building strong payer relationships, you can streamline the process and start reaping the benefits of your new contracts sooner.
Partner with WWS to optimize your credentialing process and ensure successful payer onboarding—schedule your consultation today!




