Introduction
Credentialing errors, even small ones, can have significant consequences, from delayed reimbursements to compliance violations. Learning from common mistakes can help DME providers avoid pitfalls, streamline their processes, and maintain strong payer relationships.
In this blog, we’ll examine real-world credentialing mistakes, their impact, and actionable strategies to prevent them in your practice.
Real-World Credentialing Mistakes and Their Consequences
- Submitting Incomplete Applications
- Case Study:
A DME provider submitted several applications missing required documents, leading to application denials and delayed network participation. - Impact:
Revenue loss due to inability to bill for services. - Solution:
Implement a pre-submission checklist to verify all required documents and information are included.
- Case Study:
- Missing Renewal Deadlines
- Case Study:
A provider failed to renew a key license on time, resulting in temporary delisting from a major payer network. - Impact:
Service disruptions and claims denials during the delisting period. - Solution:
Use credentialing software with automated reminders to track and prioritize renewal deadlines.
- Case Study:
- Ignoring Payer-Specific Requirements
- Case Study:
A practice used a generic application template for all payers, resulting in multiple rejections for not meeting payer-specific criteria. - Impact:
Increased administrative workload and longer credentialing timelines. - Solution:
Develop payer-specific workflows and checklists tailored to individual requirements.
- Case Study:
- Failing to Track Application Statuses
- Case Study:
Without a tracking system, a credentialing team overlooked stalled applications, delaying approvals for several months. - Impact:
Delayed reimbursements and strained payer relationships. - Solution:
Implement tracking tools to monitor application progress and schedule regular follow-ups with payers.
- Case Study:
- Lack of Internal Communication
- Case Study:
A provider’s billing team was unaware that a new hire wasn’t yet credentialed, resulting in multiple claims denials. - Impact:
Administrative inefficiencies and financial loss. - Solution:
Foster collaboration between credentialing, billing, and compliance teams to ensure seamless operations.
- Case Study:
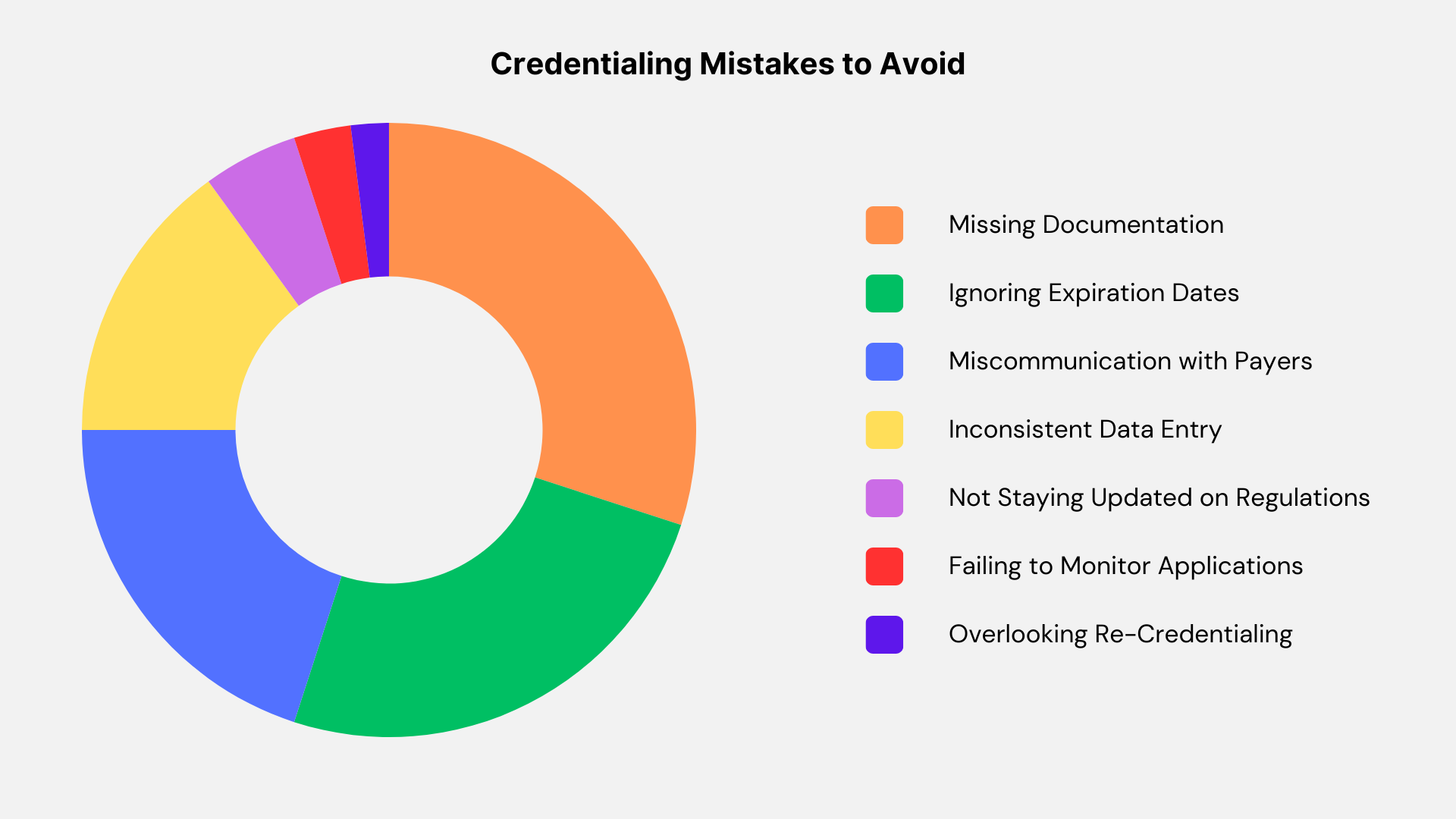
Strategies to Avoid Credentialing Mistakes
- Centralize Provider Records
- Why It Works:
Ensures all documents are complete, accurate, and easily accessible. - How to Do It:
Use a credentialing management platform to store licenses, certifications, and payer-specific forms.
- Why It Works:
- Automate Key Processes
- Why It Works:
Automation reduces manual errors and ensures timely submissions. - How to Do It:
Invest in tools that send reminders for deadlines, track application statuses, and validate data completeness.
- Why It Works:
- Train Your Team Regularly
- Why It Works:
Ensures staff stay updated on payer requirements and compliance standards. - How to Do It:
Schedule periodic training sessions and provide access to up-to-date credentialing guides.
- Why It Works:
- Conduct Internal Audits
- Why It Works:
Regular reviews identify gaps and prevent recurring mistakes. - How to Do It:
Use an audit checklist to assess documentation, workflows, and compliance metrics.
- Why It Works:
- Communicate Proactively with Payers
- Why It Works:
Strong communication minimizes delays and resolves issues quickly. - How to Do It:
Assign dedicated team members to manage payer interactions and track responses.
- Why It Works:
Monitor industry trends and benchmarks to understand common challenges and best practices for avoiding credentialing errors.
How WWS Can Help
At WWS, we help DME providers avoid credentialing mistakes with:
- Streamlined Workflows: We create customized processes to meet payer requirements efficiently.
- Technology Solutions: Our platforms automate tracking, reminders, and document management to reduce errors.
- Expert Guidance: We provide training, audits, and actionable insights to strengthen your credentialing operations.
Schedule a consultation with WWS today to safeguard your practice against credentialing mistakes:
Schedule a Meeting with WWS.
Conclusion
Credentialing mistakes can have serious financial and operational repercussions, but they’re entirely avoidable with the right strategies and tools. By centralizing records, automating processes, and fostering team collaboration, your practice can ensure accuracy, efficiency, and compliance at every step.
Partner with WWS to eliminate credentialing errors and protect your revenue—schedule your consultation today!




