Answer Summary:
A signed MCO agreement alone does not guarantee payment because providers must also be actively enrolled in the state’s base Medicaid program to avoid “Provider Not Enrolled” denials. Failure to synchronize these data silos can lead to a 15-20% spike in Days Sales Outstanding (DSO) as we head into 2026. By implementing a Master Payer Index (MPI) with “State Enrollment” gatekeepers, DME providers can eliminate these “ghost contracts” and protect their revenue from immediate recoupment risks.
The Scenario: A Premature Celebration
In the world of Revenue Cycle Management (RCM), a signed contract is usually the finish line. The hard work of negotiation is done, the rates are set, and the “In-Network” flag is raised.
This was the exact scenario for “Summit Healthcare” (anonymized), a growing provider organization expanding its footprint into South Carolina. Their contracting team successfully negotiated an agreement with Absolute Total Care, a major Medicaid Managed Care Organization (MCO) in the region. The contract was signed, the effective date was set, and the RCM team immediately loaded the payer into their billing system as “Active.”
Anticipating a surge in Medicaid volume, they began seeing patients and submitting claims. The team was confident. The paperwork was done.
Thirty days later, the denials started rolling in.
The Operational Failure
The denials weren’t for incorrect coding or lack of medical necessity. They were for “Provider Not Enrolled.”
The RCM team was baffled. They pulled the contract. It was valid. They called the MCO. The MCO confirmed they were in-network. So, why was the money not moving?
Our operational audit revealed a critical “Ghost Contract” scenario. While Summit Healthcare had successfully contracted with the Managed Care Organization, they had neglected one foundational step: State-Level Medicaid Enrollment.
In many states, including South Carolina, you cannot bill a Medicaid MCO—even with a valid contract—unless you are actively enrolled with the state’s base Medicaid program. The MCO’s claims system cross-references the state’s master provider file. If your NPI isn’t active at the state level, you are a ghost. You exist on the MCO’s contract, but you do not exist in the state’s payment ecosystem.
The financial impact was immediate and severe. Not only were new claims being denied, but the provider also faced a significant recoupment risk for any claims that had slipped through the system and been paid in error.
The Root Cause: Data Silos
The failure wasn’t just a knowledge gap; it was a structural one.
- The Provider Enrollment Team (Contracting) knew the state enrollment was pending.
- The RCM Team (Billing) only looked at the MCO contract status.
- Because these two teams worked from different data sources, the RCM team proceeded to bill a payer that was legally unbillable.
The WWS Solution: The Master Payer Index (MPI)
To fix this, Wonder Worth Solutions (WWS) didn’t just clean up the enrollment; we re-engineered the data flow. We implemented the Master Payer Index (MPI) Protocol (formerly known as the Single Source of Truth).
1. The “State Enrollment” Gatekeeper
We redesigned the central payer database to include a mandatory field: “State Enrollment Status.” This field is no longer optional. Before any Medicaid MCO—whether it’s BlueChoice or Absolute Total Care—can be marked as “Active,” the team must verify the status of the underlying state Medicaid ID.
2. The “Do Not Proceed” Logic
We utilized the “Notes” field in the MPI to create a hard stop. If the State Enrollment status is listed as “Pending” or “Inactive,” the system explicitly flags the MCO plan with a “DO NOT PROCEED” warning. This effectively blocks the RCM team from submitting claims, protecting the provider from creating a backlog of inevitable denials.
3. The Cross-Reference Protocol
We instituted a new Standard Operating Procedure (SOP). Before updating any payer status, the Provider Enrollment team must now cross-reference the payer’s online provider directory. If the provider does not appear in the public directory, the contract is considered “operationally inactive,” regardless of the signature date.
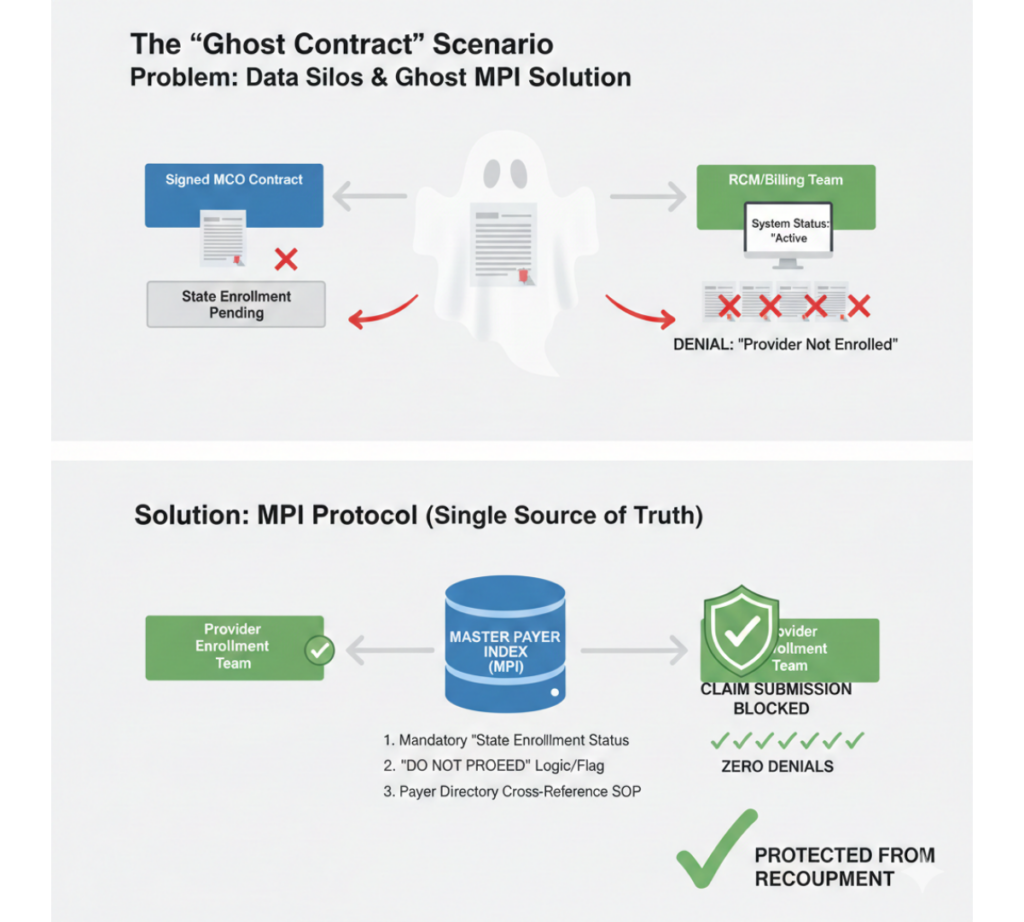
The Outcome
Since implementing the MPI Protocol, Summit Healthcare has seen zero “Unenrolled” denials for Medicaid MCOs in Q4. By forcing the RCM and Enrollment teams to look at the same “truth,” we eliminated the risk of “Ghost Contracts” and protected the client from the nightmare of a state-level recoupment audit.




