Introduction
As the healthcare industry shifts toward value-based care (VBC), the credentialing process is evolving to align with new priorities. For DME providers, this means demonstrating not only compliance but also a commitment to delivering quality outcomes and cost-effective care. Adapting your credentialing workflows to meet the demands of value-based care is critical for maintaining payer relationships and staying competitive.
In this blog, we’ll explore how credentialing requirements are changing in a value-based care environment and provide actionable strategies to adapt your processes.
How Value-Based Care Impacts Credentialing
- Emphasis on Quality Metrics
Payers are increasingly focused on outcomes and patient satisfaction, requiring providers to document and report performance metrics. - Integration Across Care Networks
Credentialing now involves coordination with other providers and organizations within integrated care models. - Greater Scrutiny of Provider Qualifications
Payers demand detailed verification of provider expertise, training, and ability to deliver value-based outcomes. - Alignment with New Contracting Models
Credentialing processes must account for bundled payments, shared savings agreements, and other value-based payment structures.
Challenges of Credentialing in a Value-Based Care Model
- Tracking Quality and Outcome Metrics
- Challenge: Providers must track and report data like readmission rates, patient satisfaction scores, and cost-efficiency.
- Solution:
Use credentialing software integrated with analytics tools to track and report these metrics accurately.
- Coordinating Across Multi-Provider Networks
- Challenge: Credentialing involves verifying relationships and roles within Accountable Care Organizations (ACOs) or other integrated networks.
- Solution:
Centralize credentialing data to streamline collaboration with other network providers.
- Adjusting to New Payer Requirements
- Challenge: Each payer’s approach to value-based care may have unique credentialing standards.
- Solution:
Develop payer-specific workflows to address varying requirements for quality measures and reporting.
- Maintaining Compliance with Traditional Standards
- Challenge: Providers must balance value-based care metrics with ongoing compliance with traditional credentialing criteria.
- Solution:
Conduct regular audits to ensure both sets of standards are consistently met.
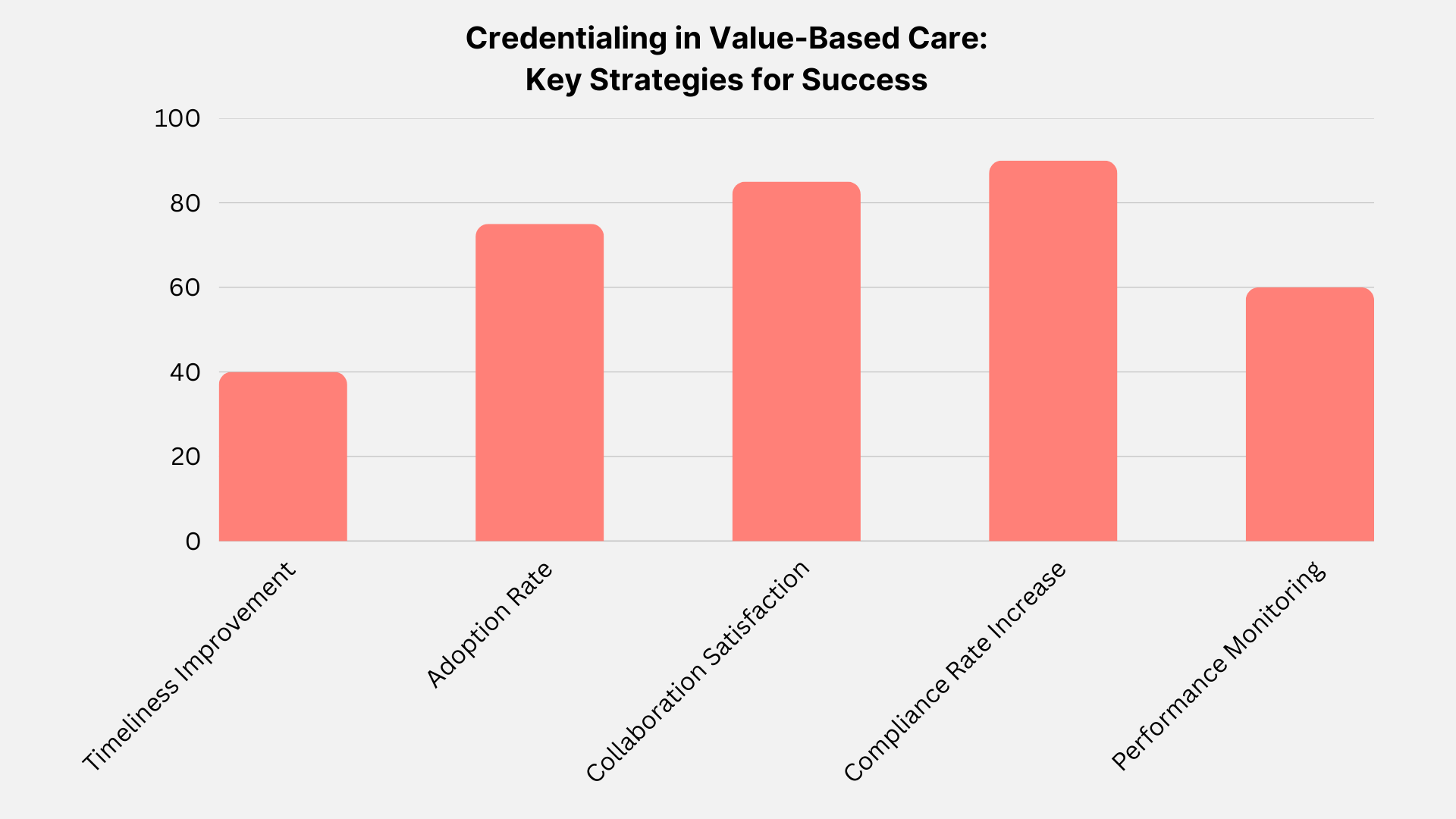
Strategies for Credentialing Success in Value-Based Care
- Focus on Quality Documentation
- Why It Works:
Thorough documentation supports your ability to meet payer expectations for quality metrics. - How to Do It:
Develop templates for capturing outcomes data and integrate them into your credentialing process.
- Why It Works:
- Collaborate Within Care Networks
- Why It Works:
Effective collaboration ensures seamless credentialing across multiple providers and organizations. - How to Do It:
Establish clear communication channels and data-sharing protocols with network partners.
- Why It Works:
- Leverage Technology to Track Metrics
- Why It Works:
Advanced tools simplify the tracking and reporting of value-based care outcomes. - How to Do It:
Use credentialing software with built-in analytics and reporting features to monitor performance.
- Why It Works:
- Train Your Team on Value-Based Care Standards
- Why It Works:
A well-informed team ensures your credentialing process aligns with evolving payer expectations. - How to Do It:
Provide regular training on value-based care principles, payer-specific requirements, and quality metrics.
- Why It Works:
- Conduct Regular Reviews of Contracts and Requirements
- Why It Works:
Staying updated on new payer agreements helps you proactively adjust your credentialing workflows. - How to Do It:
Schedule quarterly reviews of payer contracts and standards to ensure compliance and readiness.
- Why It Works:
Focus on metrics most relevant to your payers and patient population, such as equipment utilization rates, cost savings, or patient satisfaction scores.
How WWS Can Help
At WWS, we help DME providers adapt to the demands of value-based care with:
- Customized Credentialing Workflows: Tailored processes that align with value-based care requirements.
- Integrated Reporting Tools: Track and report quality metrics seamlessly through advanced credentialing platforms.
- Compliance Expertise: Ensure adherence to both traditional and value-based care standards.
Schedule a consultation with WWS today to optimize your credentialing for value-based care:
Schedule a Meeting with WWS.
Conclusion
Credentialing in a value-based care environment requires a proactive approach to tracking quality metrics, collaborating across networks, and meeting evolving payer expectations. By adapting your workflows and leveraging advanced tools, your practice can stay compliant and competitive in this new healthcare landscape.
Partner with WWS to streamline credentialing in a value-based care model—schedule your consultation today!




