Introduction
Credentialing is a dynamic process, and understanding its performance requires robust reporting. For DME providers, tracking the right metrics can uncover inefficiencies, support decision-making, and ensure compliance. Advanced reporting tools provide actionable insights into application timelines, error rates, and payer-specific trends, empowering you to optimize workflows and improve outcomes.
In this blog, we’ll explore key metrics to include in your credentialing reports and how advanced reporting can transform your operations.
Why Advanced Reporting Is Essential for Credentialing
- Enhances Visibility
Comprehensive reports provide a clear overview of credentialing workflows, highlighting areas for improvement. - Drives Data-Informed Decisions
Real-time insights allow you to allocate resources effectively and address bottlenecks. - Tracks Compliance
Monitoring credentialing data ensures adherence to payer and regulatory standards, reducing risks. - Strengthens Payer Relationships
Accurate reporting demonstrates your commitment to quality, fostering trust with payers.
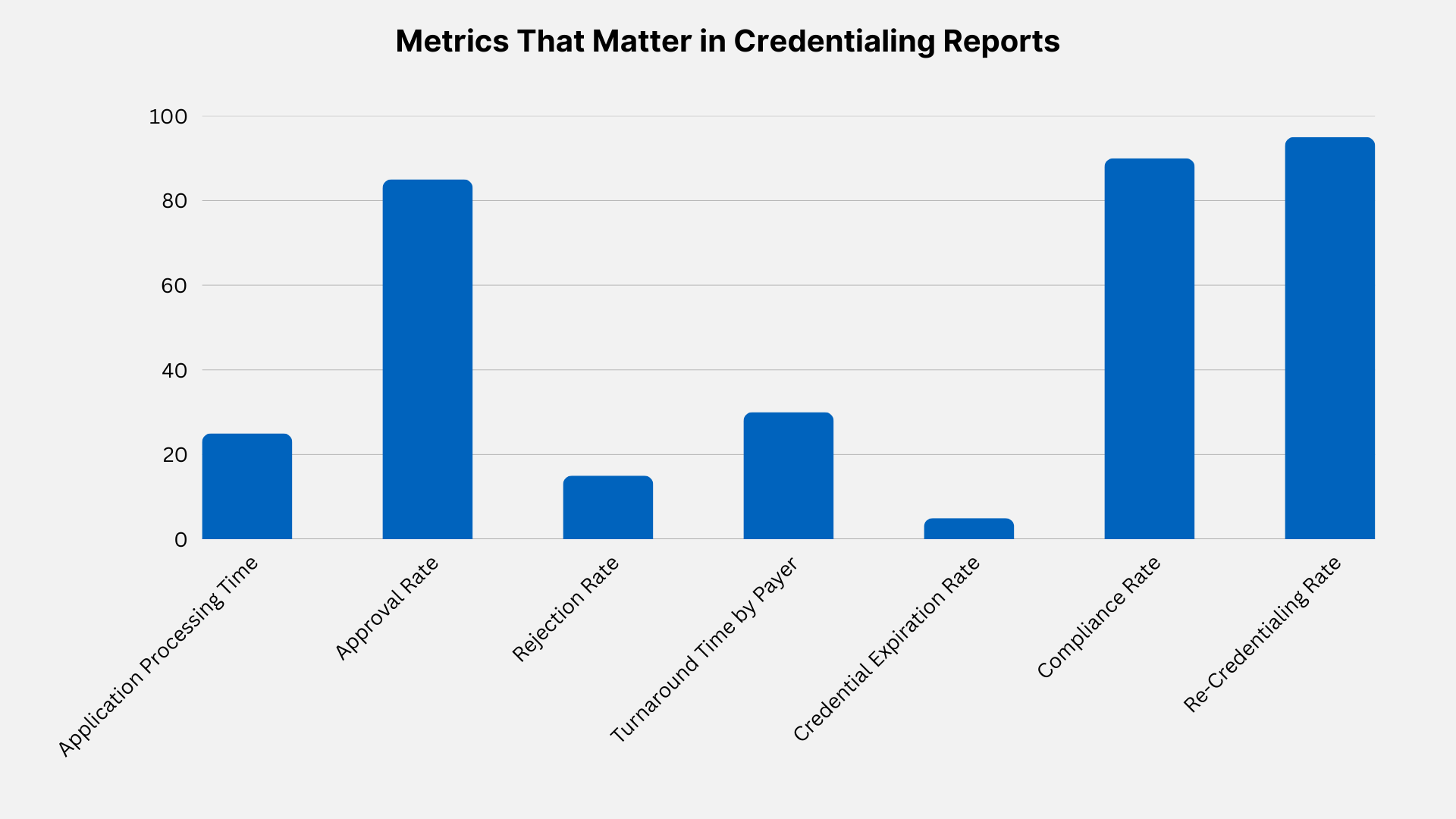
Key Metrics to Track in Credentialing Reports
- Application Approval Rates
- What It Measures:
The percentage of credentialing applications approved on the first submission. - Why It Matters:
High approval rates indicate efficient workflows and accurate documentation.
- What It Measures:
- Average Time to Credential
- What It Measures:
The time it takes to complete the credentialing process, from submission to approval. - Why It Matters:
Identifying delays helps you streamline processes and reduce turnaround times.
- What It Measures:
- Denial and Rejection Rates
- What It Measures:
The percentage of applications denied or sent back for revisions. - Why It Matters:
High rejection rates highlight gaps in preparation and documentation accuracy.
- What It Measures:
- Claims Denials Due to Credentialing Errors
- What It Measures:
The number or percentage of claims denied due to credentialing-related issues. - Why It Matters:
Understanding the financial impact of credentialing errors helps prioritize improvements.
- What It Measures:
- Payer-Specific Turnaround Times
- What It Measures:
Average credentialing timelines for each payer. - Why It Matters:
Identifies payers with slower processes, allowing for targeted follow-ups.
- What It Measures:
- Provider Credentialing Costs
- What It Measures:
The total cost of credentialing activities divided by the number of providers. - Why It Matters:
Helps identify cost-saving opportunities and optimize resource allocation.
- What It Measures:
- Compliance Metrics
- What It Measures:
Success rates in meeting regulatory standards and passing audits. - Why It Matters:
Ensures your practice is always prepared for payer reviews or regulatory inspections.
- What It Measures:
How Advanced Reporting Improves Credentialing Operations
- Identifies Bottlenecks
Benefit:- Reports highlight where applications are stalled, enabling targeted interventions.
- Enhances Accuracy
Benefit:- Tracking error trends helps refine workflows and reduce denials or delays.
- Supports Goal Setting
Benefit:- Clear metrics allow you to set realistic goals for approval rates, timelines, and compliance.
- Improves Accountability
Benefit:- Reports provide transparency, ensuring all team members understand their performance and responsibilities.
- Facilitates Benchmarking
Benefit:- Comparing performance over time or against industry standards drives continuous improvement.
Tips for Effective Credentialing Reporting
- Customize Reports to Your Needs
Tailor reports to focus on metrics that align with your practice’s goals and challenges. - Use Visual Data Representations
Charts, graphs, and dashboards make it easier to interpret data and communicate findings. - Automate Report Generation
Automated tools save time and ensure consistency in reporting. - Schedule Regular Reviews
Evaluate reports monthly or quarterly to identify trends and address issues promptly. - Share Insights Across Teams
Distribute reports to credentialing, billing, and compliance teams to foster collaboration and accountability.
Invest in reporting tools that offer real-time updates and customizable dashboards to monitor performance metrics on demand.
How WWS Can Help
At WWS, we empower DME providers with advanced reporting solutions:
- Customizable Dashboards: Track critical metrics in real-time with tailored visualizations.
- Automation Tools: Simplify report generation and ensure consistent, error-free insights.
- Expert Analysis: We help you interpret data and identify actionable steps for improvement.
Schedule a consultation with WWS today to unlock the power of advanced credentialing reporting:
Schedule a Meeting with WWS.
Conclusion
Advanced reporting is a game-changer for credentialing, providing the insights needed to optimize workflows, improve compliance, and reduce errors. By tracking the right metrics and leveraging data-driven tools, your practice can enhance efficiency and strengthen payer relationships.
Partner with WWS to transform your credentialing process with advanced reporting—schedule your consultation today!




