Introduction
For DME providers, credentialing with multiple payers is often a necessity to maximize patient access and diversify revenue streams. However, the complexity of managing different requirements, timelines, and documentation can quickly become overwhelming. Without a streamlined approach, multi-payer credentialing can lead to errors, delays, and missed opportunities.
In this blog, we’ll explore strategies for simplifying multi-payer credentialing, helping you stay organized and efficient while meeting each payer’s unique expectations.
The Challenges of Multi-Payer Credentialing
- Varying Requirements Across Payers
Each payer has distinct credentialing criteria, including documentation, timelines, and verification processes. - Overlapping Deadlines
Managing multiple re-credentialing or renewal deadlines can lead to missed submissions and disruptions in network participation. - Complex Communication
Coordinating with multiple payer representatives to track application statuses and resolve issues is time-intensive. - Risk of Errors
Handling multiple credentialing workflows manually increases the likelihood of documentation errors or incomplete applications.
Best Practices for Streamlining Multi-Payer Credentialing
- Centralize Credentialing Records
- Why It Works:
A centralized system simplifies access to provider documentation and ensures consistency across applications. - How to Do It:
Use credentialing software to store all provider records in one secure, organized platform.
- Why It Works:
- Create Payer-Specific Workflows
- Why It Works:
Tailored workflows help you meet each payer’s unique requirements without confusion. - How to Do It:
Develop checklists for each payer, detailing required documents, submission processes, and key contacts.
- Why It Works:
- Automate Deadline Tracking
- Why It Works:
Automated reminders prevent missed renewals and help prioritize high-value payers. - How to Do It:
Implement a credentialing management system that tracks deadlines and sends alerts for upcoming expirations.
- Why It Works:
- Standardize Application Preparation
- Why It Works:
Standardized templates reduce errors and speed up application preparation for multiple payers. - How to Do It:
Create uniform templates for commonly requested documents, such as licenses, certifications, and insurance details.
- Why It Works:
- Assign Dedicated Payer Specialists
- Why It Works:
Focused attention on specific payers ensures better communication and faster issue resolution. - How to Do It:
Assign team members to manage individual payers, building expertise and fostering stronger relationships.
- Why It Works:
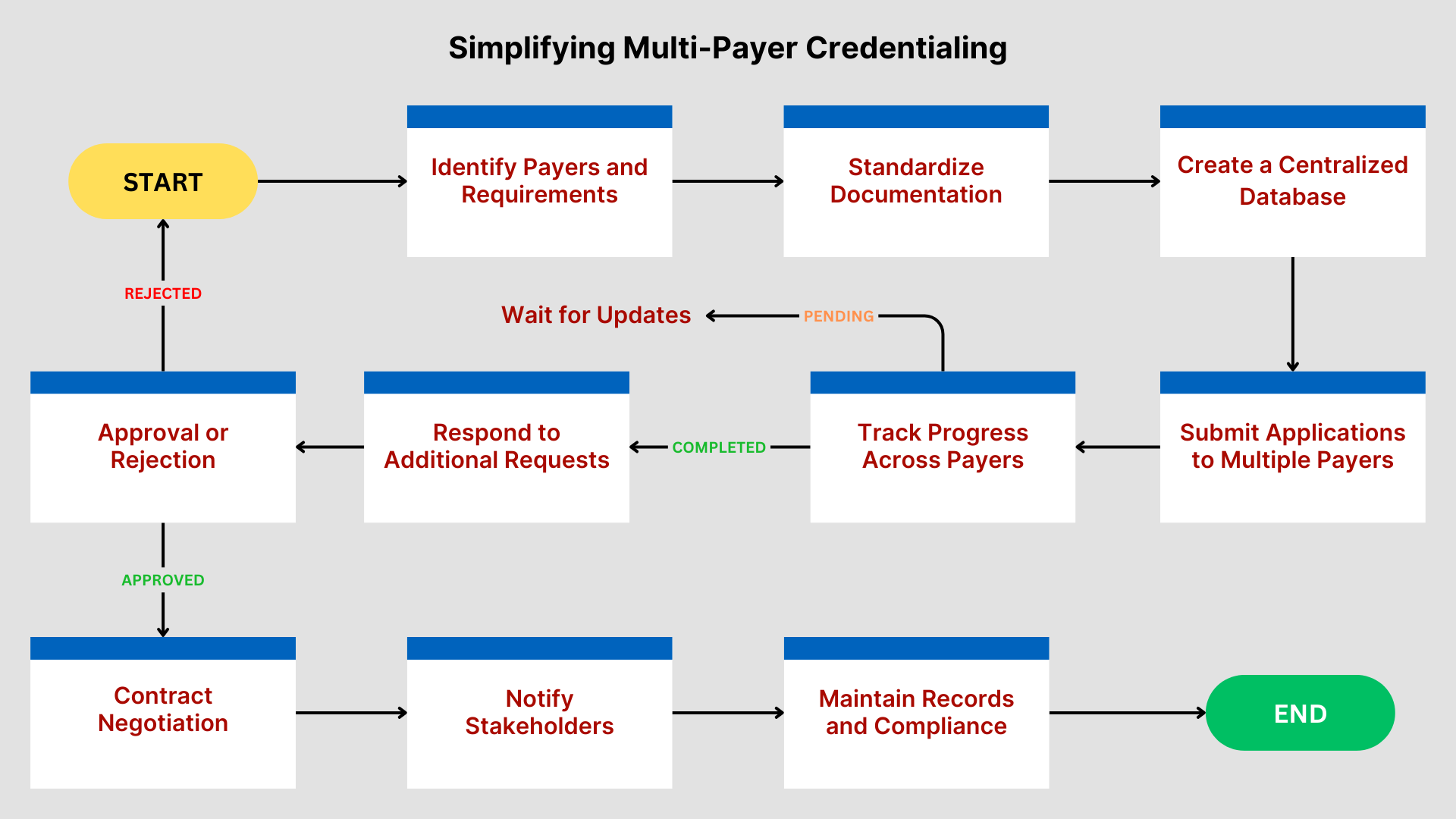
Common Pitfalls to Avoid in Multi-Payer Credentialing
- Overlooking Payer Updates
- Pitfall: Missing changes to credentialing requirements or processes leads to delays.
- Solution: Regularly review payer communications and update workflows accordingly.
- Failing to Track Statuses
- Pitfall: Applications stall when there’s no follow-up on pending approvals.
- Solution: Use tracking tools to monitor progress and schedule regular follow-ups with payers.
- Rushing to Meet Deadlines
- Pitfall: Last-minute submissions often contain errors or missing documents.
- Solution: Plan submissions well in advance and conduct pre-submission audits to ensure accuracy.
Focus your resources on payers that represent the largest share of your revenue or patient population to minimize disruptions and maximize returns.
How WWS Can Help
Navigating multi-payer credentialing doesn’t have to be overwhelming. At WWS, we provide:
- Centralized Credentialing Management: Our systems keep all provider records organized and accessible for streamlined submissions.
- Tailored Workflows: We create payer-specific strategies to meet unique requirements efficiently.
- Automation Tools: From tracking deadlines to automating reminders, our tools help you stay on top of every credentialing task.
- Expert Support: Our team handles communication and issue resolution with payers, so you don’t have to.
Schedule a consultation with WWS today to simplify your multi-payer credentialing process:
Schedule a Meeting with WWS.
Conclusion
Multi-payer credentialing is complex, but with the right strategies, tools, and support, you can streamline the process and maintain compliance across networks. By centralizing records, automating workflows, and fostering payer relationships, you can ensure your practice stays competitive and efficient.
Partner with WWS to optimize your multi-payer credentialing—schedule your consultation today!




