Introduction
Credentialing errors aren’t just administrative hiccups—they directly affect your bottom line. From claim denials to delayed reimbursements, even minor mistakes can disrupt cash flow and increase operational costs.
In this blog, we’ll explore the financial impact of credentialing errors, identify common causes, and provide actionable strategies to prevent them, ensuring a smoother revenue cycle for your DME practice.
The Financial Impact of Credentialing Errors
- Increased Claim Denials
- How It Happens:
Claims submitted by uncredentialed or incorrectly credentialed providers are rejected by payers. - Financial Impact:
Lost revenue, additional administrative costs to resubmit claims, and potential delays in patient care.
- How It Happens:
- Payment Delays
- How It Happens:
Credentialing errors stall payer approvals, delaying the ability to bill for services. - Financial Impact:
Disrupted cash flow, leading to difficulty covering operational expenses.
- How It Happens:
- Re-Credentialing Costs
- How It Happens:
Errors in re-credentialing applications require time-consuming corrections and rework. - Financial Impact:
Increased administrative workload and longer approval timelines.
- How It Happens:
- Payer Network Delisting
- How It Happens:
Repeated credentialing issues can result in being dropped from payer networks. - Financial Impact:
Loss of access to patient populations and significant revenue streams.
- How It Happens:
Common Causes of Credentialing Errors
- Incomplete or Incorrect Documentation
Missing or outdated provider licenses, certifications, or insurance details can lead to application rejections. - Missed Deadlines
Failing to submit re-credentialing applications on time causes temporary delisting and billing interruptions. - Lack of Payer-Specific Knowledge
Generic credentialing workflows fail to account for unique requirements across payers, resulting in non-compliance. - Manual Tracking Errors
Reliance on spreadsheets or paper systems increases the risk of oversights and inaccuracies. - Inadequate Team Training
Staff unfamiliar with credentialing processes are more likely to make errors in applications or documentation.
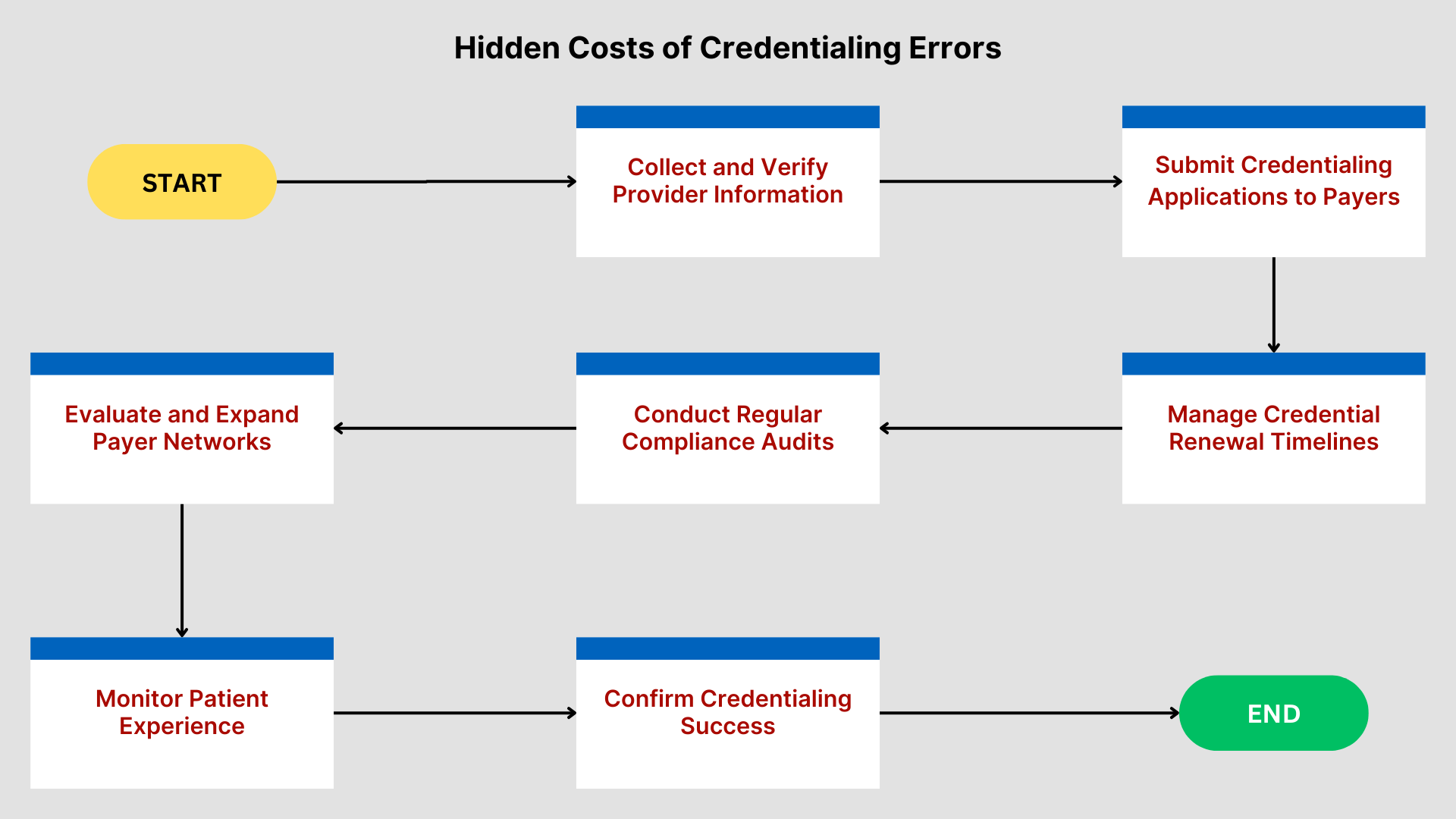
Preventing Credentialing Errors
- Centralize Provider Documentation
- Why It Works:
Keeps all licenses, certifications, and other required documents up-to-date and accessible. - How to Do It:
Use a credentialing management platform to store and organize records securely.
- Why It Works:
- Automate Tracking and Deadlines
- Why It Works:
Reduces human error and ensures timely submissions for credentialing and re-credentialing. - How to Do It:
Implement software that sends automatic reminders for expirations and application deadlines.
- Why It Works:
- Customize Workflows for Payers
- Why It Works:
Ensures compliance with each payer’s specific requirements. - How to Do It:
Develop payer-specific credentialing checklists and assign dedicated team members to manage key accounts.
- Why It Works:
- Conduct Pre-Submission Audits
- Why It Works:
Identifies errors before applications are sent, reducing the risk of denials or delays. - How to Do It:
Review all applications for completeness and accuracy before submission.
- Why It Works:
- Invest in Staff Training
- Why It Works:
Reduces errors by ensuring staff understand credentialing processes and payer expectations. - How to Do It:
Provide ongoing education on industry updates, compliance standards, and credentialing tools.
- Why It Works:
How WWS Can Help
At WWS, we help DME providers eliminate credentialing errors and optimize reimbursements:
- Automation Solutions: Our tools streamline workflows, track deadlines, and reduce manual errors.
- Customized Payer Workflows: We tailor credentialing processes to meet the unique requirements of each payer.
- Comprehensive Support: From pre-submission audits to staff training, we ensure your credentialing process is error-free and efficient.
Schedule a consultation with WWS today to safeguard your reimbursements and streamline credentialing:
Schedule a Meeting with WWS.
Conclusion
Credentialing errors can have a significant financial impact, but they’re entirely preventable with the right tools and strategies. By centralizing documentation, automating workflows, and investing in staff training, you can ensure a seamless credentialing process and protect your revenue cycle.
Partner with WWS to eliminate credentialing errors and maximize your reimbursements—schedule your consultation today!




