Introduction
Provider turnover is an inevitable challenge for DME practices. Whether onboarding new providers or managing the departure of existing ones, credentialing during these transitions is critical to maintaining compliance and avoiding disruptions in service delivery and revenue.
In this blog, we’ll explore the key challenges of credentialing during provider turnover and share actionable strategies to ensure seamless transitions while maintaining operational continuity.
The Impact of Provider Turnover on Credentialing
- Risk of Credentialing Gaps
Turnover can lead to lapses in provider credentials, resulting in billing interruptions or payer delisting. - Increased Administrative Workload
Managing credentialing for departing and incoming providers adds to the administrative burden. - Potential for Errors and Delays
The rush to credential new providers or manage transitions can result in incomplete applications or missed deadlines. - Compliance Challenges
Ensuring all licensing, payer enrollment, and documentation requirements are met during transitions can strain resources.
Challenges in Credentialing During Provider Turnover
- Onboarding New Providers Quickly
- Challenge: Delays in credentialing new hires impact their ability to see patients and bill payers.
- Solution:
Start credentialing during the hiring process and use automation to expedite submissions.
- Managing Departing Provider Responsibilities
- Challenge: Uncredentialed replacements may not be able to take over patient care or billing responsibilities immediately.
- Solution:
Overlap credentialing timelines to ensure continuity of care and reimbursement.
- Updating Payer Networks
- Challenge: Failure to update payers about provider changes can lead to compliance issues or claims rejections.
- Solution:
Notify payers promptly and provide necessary documentation for updates.
- Handling Increased Documentation Requirements
- Challenge: Collecting, verifying, and managing documentation for multiple transitions strains administrative resources.
- Solution:
Centralize documentation management to streamline the process.
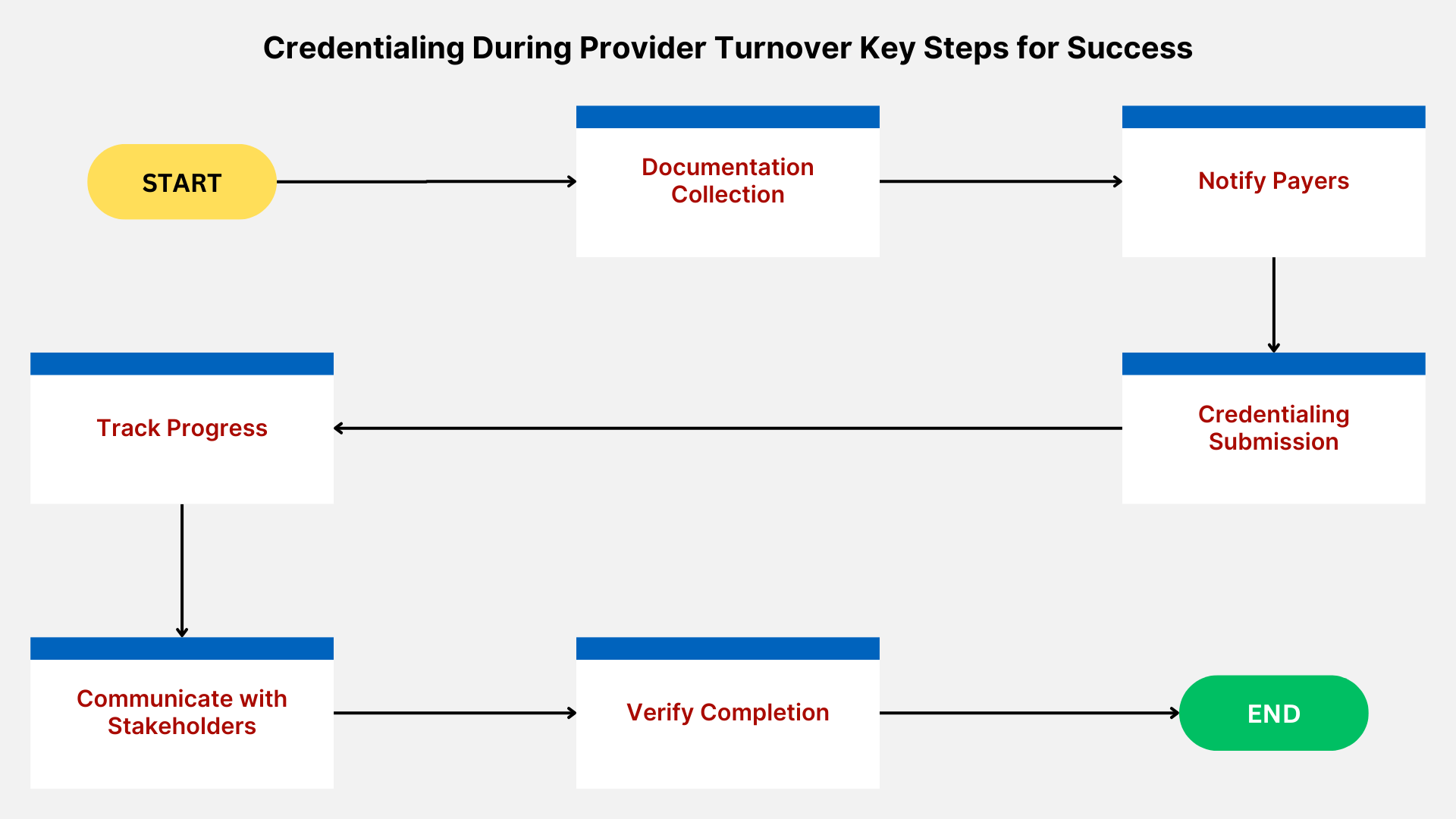
Strategies for Seamless Credentialing During Provider Turnover
- Create a Turnover Credentialing Checklist
- Why It Works:
A structured checklist ensures all steps are completed for both departing and incoming providers. - How to Do It:
Include items like payer notifications, license verifications, and documentation updates.
- Why It Works:
- Start Early for New Hires
- Why It Works:
Initiating credentialing during onboarding reduces delays. - How to Do It:
Begin collecting documentation and submitting applications as soon as the hiring process begins.
- Why It Works:
- Overlap Credentialing Timelines
- Why It Works:
Overlapping ensures that replacements are ready to take over responsibilities without interruptions. - How to Do It:
Coordinate credentialing timelines for departing and incoming providers to minimize gaps.
- Why It Works:
- Automate Documentation and Tracking
- Why It Works:
Automation reduces errors and ensures deadlines are met. - How to Do It:
Use credentialing software to track provider statuses, manage deadlines, and send reminders.
- Why It Works:
- Communicate Clearly with Payers
- Why It Works:
Timely communication ensures network updates are processed smoothly. - How to Do It:
Assign a dedicated team member to handle payer notifications and follow-ups.
- Why It Works:
Prepare a cross-trained credentialing team that can handle increased workloads during provider transitions without sacrificing accuracy.
How WWS Can Help
At WWS, we simplify credentialing during provider turnover with:
- Comprehensive Turnover Workflows: Tailored strategies to ensure smooth transitions for departing and incoming providers.
- Automation Tools: Streamline tracking, submissions, and documentation management for turnover scenarios.
- Payer Communication Support: Ensure timely updates and approvals with expert liaison services.
Schedule a consultation with WWS today to manage credentialing during provider turnover seamlessly:
Schedule a Meeting with WWS.
Conclusion
Provider turnover doesn’t have to disrupt your operations or compliance. By starting credentialing early, automating workflows, and maintaining clear communication with payers, your practice can navigate transitions effectively and maintain service continuity.
Partner with WWS to streamline credentialing during provider turnover—schedule your consultation today!




