Introduction
Credentialing errors may seem like minor missteps, but they can have far-reaching financial and operational consequences for DME providers. From denied claims to compliance penalties, these mistakes can quietly drain your resources and impact patient care.
In this blog, we’ll uncover the hidden costs of credentialing errors, explore common pitfalls, and provide actionable strategies to avoid them, ensuring your credentialing process supports profitability and compliance.
The True Cost of Credentialing Errors
- Lost Revenue from Claim Denials
- The Impact:
Claims submitted by uncredentialed providers are automatically denied, leading to delayed reimbursements or lost revenue. - How to Avoid:
- Verify provider credentials before submitting claims.
- Integrate credentialing systems with billing platforms to flag potential issues.
- The Impact:
- Increased Administrative Workload
- The Impact:
Correcting errors requires resubmitting applications, tracking updates, and coordinating with payers, consuming valuable staff time. - How to Avoid:
Use credentialing management software to streamline application tracking and reduce manual work.
- The Impact:
- Payer Network Delisting
- The Impact:
Errors in re-credentialing or missed deadlines can lead to temporary or permanent delisting, cutting off access to key revenue streams. - How to Avoid:
Automate renewal reminders and prioritize re-credentialing for high-value payers.
- The Impact:
- Compliance Penalties
- The Impact:
Inaccurate provider files or missing documentation can result in fines during payer or accreditation audits. - How to Avoid:
Conduct regular internal audits to ensure files meet compliance standards.
- The Impact:
- Damage to Reputation and Relationships
- The Impact:
Repeated errors can strain payer relationships and diminish patient trust. - How to Avoid:
Build a robust credentialing workflow and maintain proactive communication with payers.
- The Impact:
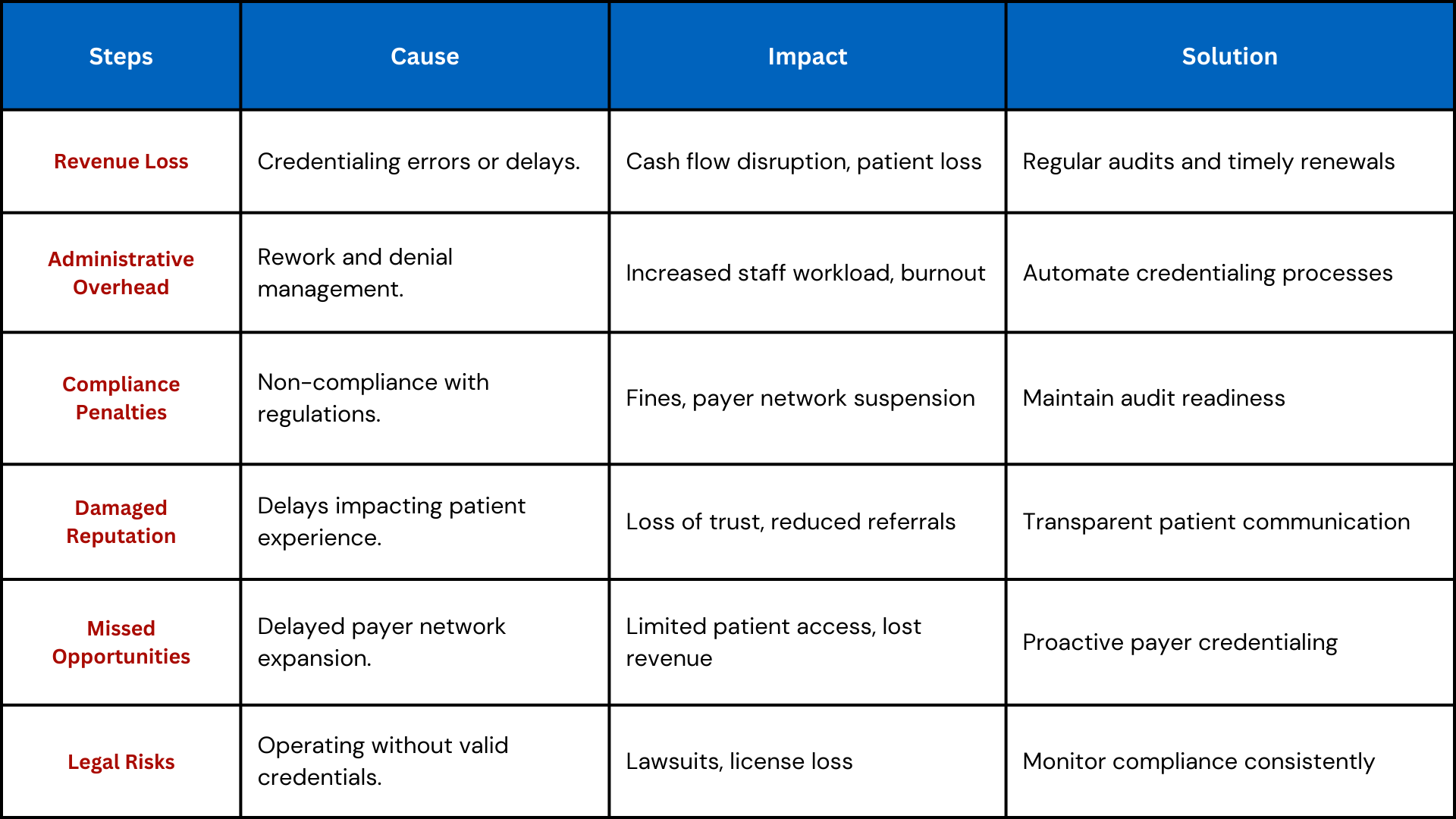
Common Credentialing Mistakes to Watch For
- Incomplete Applications
- Missing documents or inaccurate information leads to delays or rejections.
- Solution: Implement a thorough application checklist for all providers.
- Missed Deadlines
- Failure to renew licenses or re-credential on time disrupts billing and payer status.
- Solution: Use automated systems to track and remind you of critical deadlines.
- Ignoring Payer-Specific Requirements
- Submitting a generic application to all payers may result in non-compliance.
- Solution: Customize workflows to meet the unique requirements of each payer.
- Lack of Follow-Up
- Applications may stall without proactive follow-ups, extending approval timelines.
- Solution: Assign a dedicated team member to monitor and follow up on pending applications.
Strategies to Avoid Credentialing Errors
- Centralize Provider Data
- Why It Works:
Ensures all documentation is complete, accurate, and accessible. - How to Do It:
Use a secure credentialing platform to store licenses, certifications, and payer-specific forms.
- Why It Works:
- Automate Workflows
- Why It Works:
Automation reduces human error and ensures timely submissions. - How to Do It:
Implement credentialing software to automate reminders, track application progress, and flag discrepancies.
- Why It Works:
- Train Your Credentialing Team
- Why It Works:
Knowledgeable staff are less likely to make costly mistakes. - How to Do It:
Provide regular training on payer requirements, industry standards, and compliance updates.
- Why It Works:
- Conduct Pre-Submission Audits
- Why It Works:
Catching errors before submission prevents delays and denials. - How to Do It:
Review applications for completeness and accuracy before sending them to payers.
- Why It Works:
- Maintain Proactive Communication with Payers
- Why It Works:
Open lines of communication ensure you stay informed of changes and address issues quickly. - How to Do It:
Establish relationships with payer representatives and schedule regular check-ins.
- Why It Works:
How WWS Can Help
At WWS, we help DME providers eliminate credentialing errors with tailored solutions:
- Automation Tools: Our systems streamline workflows, track deadlines, and minimize human error.
- Document Management: We centralize and organize provider data for easy access and compliance.
- Proactive Support: From pre-submission audits to payer communication, our team ensures a smooth credentialing process.
Schedule a consultation with WWS today to reduce errors and optimize your credentialing operations:
Schedule a Meeting with WWS.
Conclusion
Credentialing errors can quietly erode your profitability and disrupt operations, but they’re entirely preventable with the right strategies and tools. By centralizing data, automating workflows, and training your team, you can avoid costly mistakes and maintain seamless payer relationships.
Partner with WWS to eliminate credentialing errors—schedule your consultation today!




