Introduction
Measuring the success of your credentialing processes is essential for maintaining compliance, minimizing delays, and optimizing operations. Key Performance Indicators (KPIs) provide actionable insights into your credentialing efficiency, highlighting areas for improvement and driving better outcomes.
In this blog, we’ll outline the most important credentialing KPIs for DME providers and share strategies to monitor and enhance your performance.
Why Tracking Credentialing KPIs Is Critical
- Identifies Bottlenecks
KPIs reveal process inefficiencies, helping you address delays and improve workflows. - Ensures Compliance
Monitoring metrics ensures adherence to payer and regulatory standards, reducing risks of penalties or delisting. - Enhances Payer Relationships
Strong KPI performance demonstrates reliability and fosters trust with payers. - Protects Revenue
Tracking approval rates and timelines minimizes claim denials and improves cash flow. - Supports Continuous Improvement
Regularly evaluating KPIs allows you to refine processes and achieve long-term success.
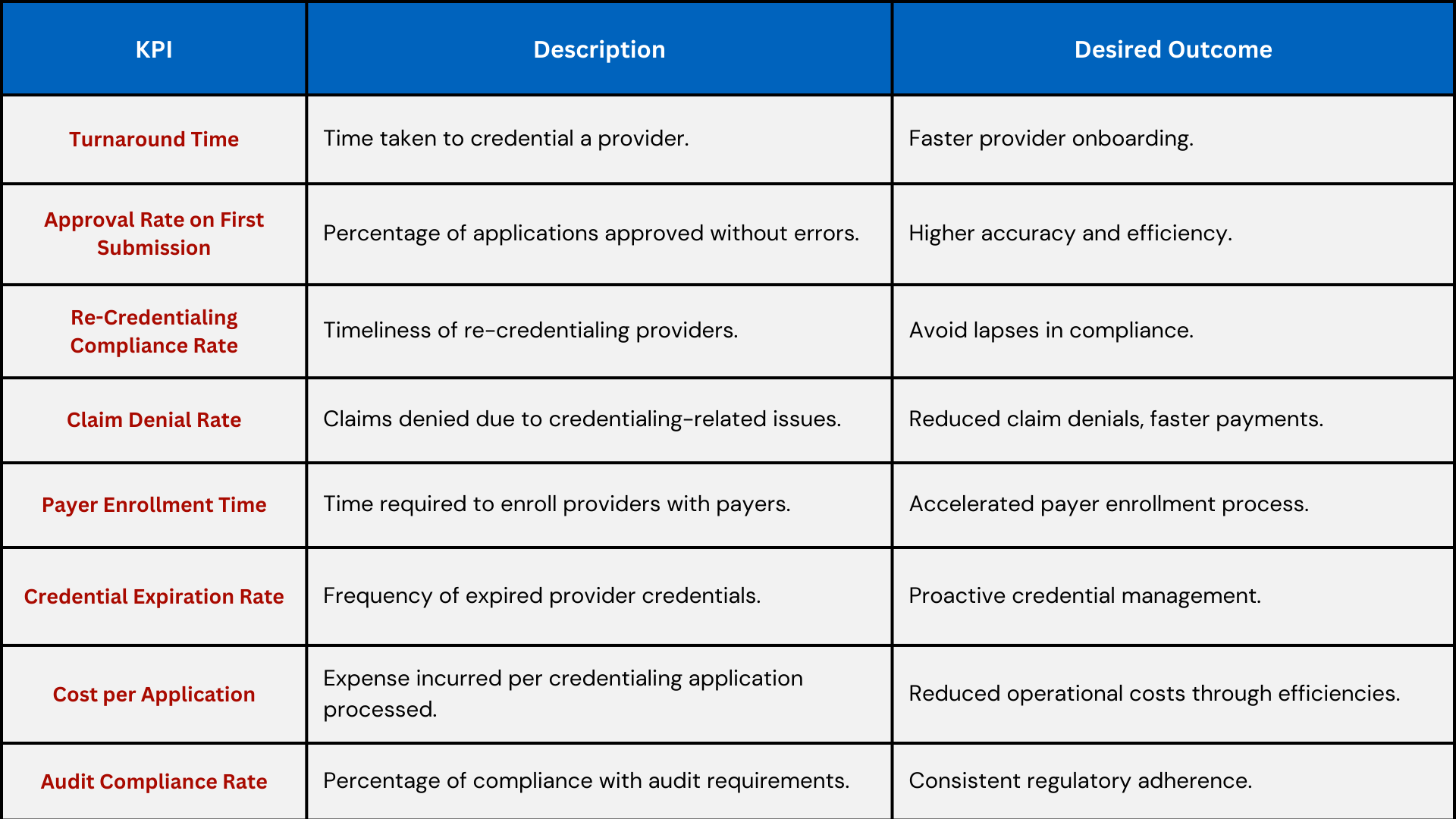
Top Credentialing KPIs for DME Providers
- Application Approval Rate
- What It Measures:
Percentage of credentialing applications approved on the first submission. - Why It Matters:
A high approval rate indicates accurate documentation and efficient workflows.
- What It Measures:
- Average Time to Credential
- What It Measures:
Time taken from application submission to approval. - Why It Matters:
Shorter timelines improve provider onboarding and revenue generation.
- What It Measures:
- Denial and Rejection Rate
- What It Measures:
Percentage of applications denied or sent back for revisions. - Why It Matters:
High rates highlight documentation errors or inconsistencies that need correction.
- What It Measures:
- Claims Denials Due to Credentialing Errors
- What It Measures:
Number or percentage of claims denied due to credentialing-related issues. - Why It Matters:
Reducing these denials protects revenue and improves payer relationships.
- What It Measures:
- Re-Credentialing Compliance Rate
- What It Measures:
Percentage of providers re-credentialed before deadlines. - Why It Matters:
Ensures uninterrupted payer participation and compliance.
- What It Measures:
- Payer-Specific Turnaround Times
- What It Measures:
Average time for credentialing approvals with individual payers. - Why It Matters:
Identifies payers with slower processes, enabling targeted follow-ups.
- What It Measures:
- Provider Credentialing Costs
- What It Measures:
Total costs of credentialing activities divided by the number of providers. - Why It Matters:
Helps identify inefficiencies and opportunities to reduce administrative expenses.
- What It Measures:
Strategies to Monitor and Improve Credentialing KPIs
- Use Real-Time Dashboards
- Why It Works:
Dashboards provide instant visibility into performance metrics and trends. - How to Do It:
Invest in credentialing software with built-in reporting and analytics features.
- Why It Works:
- Conduct Regular Performance Reviews
- Why It Works:
Reviewing KPIs regularly highlights areas for improvement. - How to Do It:
Schedule monthly or quarterly reviews with your team to discuss metrics and action plans.
- Why It Works:
- Automate Tracking and Reporting
- Why It Works:
Automation ensures accurate data collection and minimizes manual effort. - How to Do It:
Use tools that generate real-time reports and send alerts for underperforming metrics.
- Why It Works:
- Address Root Causes of Denials
- Why It Works:
Resolving common issues improves approval rates and reduces delays. - How to Do It:
Analyze denial trends and implement targeted training or process adjustments.
- Why It Works:
- Align KPIs with Organizational Goals
- Why It Works:
Focusing on relevant metrics ensures your credentialing process supports broader objectives. - How to Do It:
Collaborate with leadership to identify priority KPIs that align with your practice’s strategic goals.
- Why It Works:
Compare your KPIs to industry benchmarks to evaluate your practice’s credentialing efficiency and set realistic improvement targets.
How WWS Can Help
At WWS, we empower DME providers to monitor and enhance credentialing performance with:
- Customizable Dashboards: Track key metrics in real time with tailored visualizations.
- Automation Tools: Simplify data collection, reporting, and trend analysis.
- Expert Guidance: Identify opportunities for improvement and implement best practices for KPI success.
Schedule a consultation with WWS today to optimize your credentialing performance:
Schedule a Meeting with WWS.
Conclusion
Tracking and improving credentialing KPIs is essential for optimizing your processes, maintaining compliance, and protecting revenue. By focusing on the right metrics, leveraging technology, and fostering a culture of continuous improvement, your practice can achieve long-term success in credentialing.
Partner with WWS to elevate your credentialing performance and streamline your operations—schedule your consultation today!




